Varicocele
What is Varicocele?
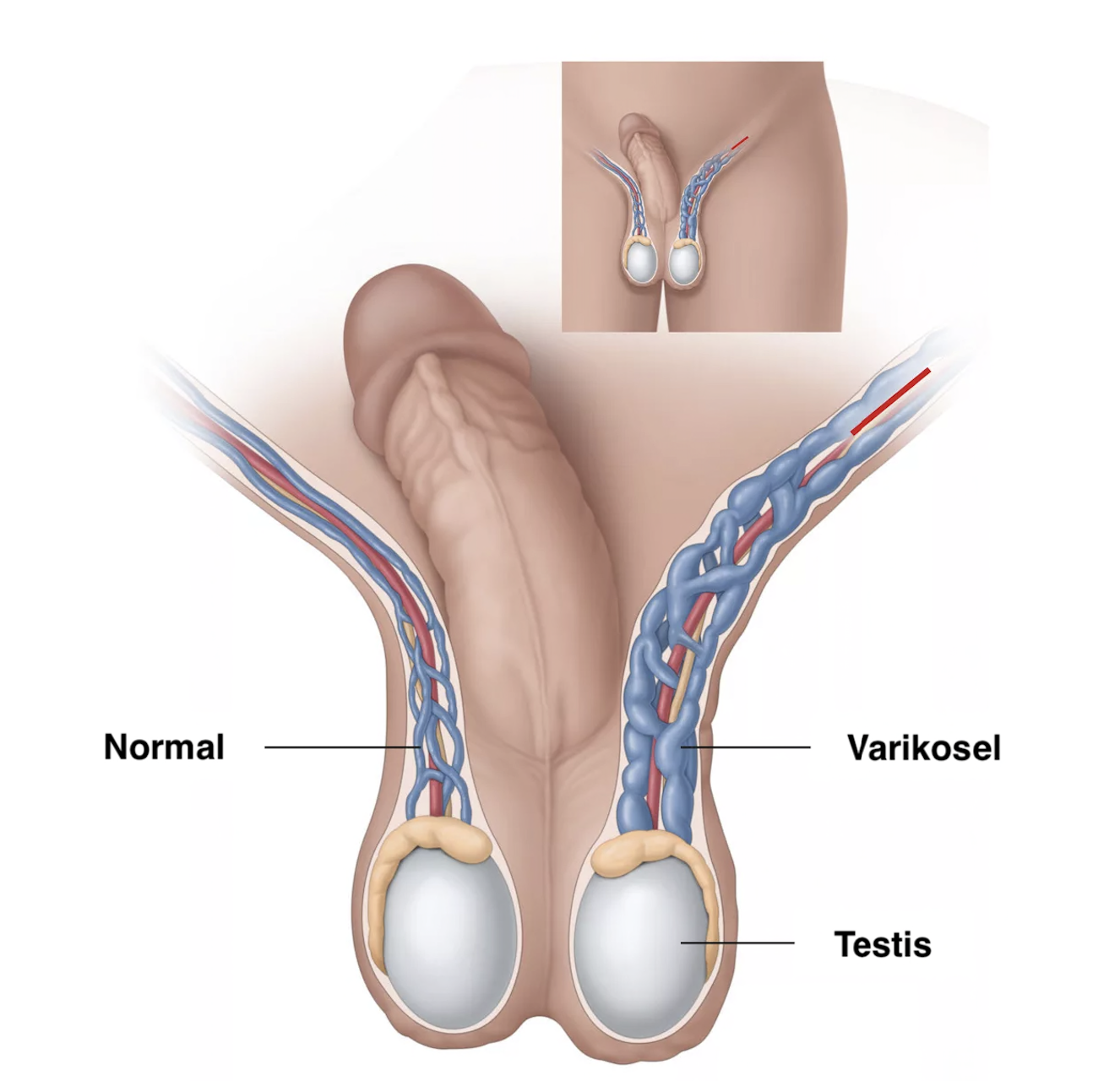
Varicocele is a condition that occurs when the veins in the testicle become varicose, or enlarged. This condition can be thought of as the testicular equivalent of varicose veins seen in the legs. Varicocele is most often noticed during adolescence or young adulthood. It usually develops gradually and is most commonly seen in the left testicle. This is because the left testicular vein is anatomically connected to the main vein at a right angle. Therefore, the pressure inside the vein is higher than on the right side.
How Does Varicocele Form?
The veins in the body carry blood back to the heart from various organs. Normally, these veins have valves that ensure blood flows in the correct direction. However, when the valves in the testicular veins do not function properly, gravity can cause blood to pool in the scrotum, resulting in varicocele.
What Are the Causes of Varicocele?
Although the exact cause of varicocele is not fully understood, the underlying mechanism is the malfunctioning of the valves in the veins. Normally, these valves ensure that blood flows in one direction towards the heart. When the valves malfunction, blood flows backwards and accumulates in the veins, causing them to dilate. Over time, this dilation creates the appearance of varicocele.
What is Adolescent Varicocele?
Adolescent varicocele usually occurs during the rapid growth period of adolescence and is rare before adolescence. It often causes no symptoms and is usually discovered by chance by the patient or doctor.
While the main goal of varicocele treatment in adults is to increase fertility, the primary objective in adolescents is to protect the testicles from potential future damage and ensure future fertility.
The diagnosis and treatment process is more complex in adolescents because the testicles grow rapidly during this period and hormone levels fluctuate constantly.
Surgery is generally recommended for varicocele in adolescents in the following situations:
- A persistent difference of more than 20% in testicular volume,
- Detection of abnormalities in semen analysis,
- Pain in the testicle and scrotum that impairs quality of life.
Studies show that normal growth is restored in the affected testicle in 60–90% of cases after surgery.
Therefore, the decision to perform surgery for adolescent varicocele should be made by evaluating multiple factors together, such as the presence of pain, testicular volume difference, semen analysis, and hormone levels.
Furthermore, before considering surgery, patients should be monitored for at least 6–12 months to observe whether spontaneous growth occurs in the testicles.
Since semen analysis is not always easily performed in adolescents, the decision for surgery is often based on changes in testicular volume.
Don't delay, let's meet now !
- Feneryolu Bagdat Avenue No 85/1 Postal Code: 34724 Kadıköy/İstanbul - Turkey
How Common is Varicocele?
Varicocele is quite common. In fact, 15% of all adult males have varicocele.
In many men, varicocele goes unnoticed throughout their lives or does not cause any problems.
Approximately 20% of adolescents also have varicocele, and some of these cases may resolve spontaneously.
What Are the Problems Associated with Varicocele?
Varicocele can lead to three main problems:
- Infertility
- Decreased testosterone production in the testicle
- Discomfort and pain in the testicle and scrotum area
In some cases, varicocele can even lead to azoospermia, meaning there are no sperm in the semen.
Varicocele is such a common condition that it sometimes goes unnoticed throughout a man's life, and approximately 80% of men with varicocele are able to conceive naturally with their partners without any medical intervention.
Furthermore, most men with varicocele can continue their lives without experiencing hormonal problems or pain or discomfort in the testicles.
How Does Varicocele Affect the Testicle?
There are several theories about how varicocele affects the testicles.
The testicles function best at a temperature approximately 2 to 4 degrees lower than body temperature. The increase in temperature caused by varicocele can negatively affect sperm and testosterone production.
Other theories include the formation of a mass effect on the testicle and exposure of the testicle to various chemicals from the adrenal gland located above the testicular vein.
Is Varicocele Dangerous?
Varicocele does not threaten life, but it can rarely be associated with dangerous conditions.
For example, if a varicocele occurs on the right side and not on the left, it is necessary to ensure that it is not caused by a mass or other abnormality in the abdomen.
Additionally, a varicocele should shrink or decrease in fullness when lying down, as gravity no longer fills the pampiniform plexus veins.
If the varicocele does not shrink, this may suggest an obstruction such as a mass or tumour in the abdomen.
Varicoceles can also affect testosterone production. However, many men with varicoceles maintain adequate testosterone levels throughout their lives without treatment.
In rare cases, varicocele can cause severe testosterone deficiency, which can lead to complications such as metabolic syndrome, diabetes, and osteoporosis.
In addition, varicoceles are one of the most common causes of male infertility.
Varicoceles can negatively affect sperm production and quality by causing a deterioration process that leads to increased heat in the testicles and damage to sperm cells.
This condition may manifest as a decrease in sperm count, reduced motility, and morphological abnormalities.
Therefore, it is important to evaluate varicocele and treat it when necessary, especially in men who are struggling to have children.
What is the "Grading" System for Varicocele Size?
Varicocele grading systems help define the size of the varicocele and guide treatment.
Various systems have been developed, but the most commonly used scale today is as follows:
- Grade 0: Visible only on ultrasound, not detectable on physical examination (subclinical varicocele)
- Grade 1: Detectable on examination when the patient performs the Valsalva manoeuvre (straining)
- Grade 2: Can be felt by hand even without straining
- Grade 3: Causes visible deformity in the scrotum
Even within Grades II and III, experienced physicians can distinguish between different sizes, and these findings can help determine whether varicocele should be treated.
Can Varicocele Cause Problems Later in Life?
Varicocele has been shown to gradually affect both fertility parameters and testosterone levels over time.
Furthermore, almost all men who undergo varicocele repair experience an increase in testosterone levels after surgery. However, this does not mean that all men with varicocele need treatment. Many men can live their entire lives without knowing they have varicocele and without experiencing any symptoms.
What Are the Symptoms of Varicocele?
Varicocele does not cause noticeable symptoms in most people and is usually detected during routine examinations. However, some patients may describe fullness, heaviness, or mild pain in the testicle that increases at the end of the day. Symptoms may become more pronounced, especially after prolonged standing or physical exertion. In advanced cases, the dilation of the veins may be visible externally, creating a "worm-like" appearance.
In men who are unable to have children, varicocele may be the underlying cause in up to 40% of cases, as it can negatively affect sperm quality. Therefore, varicocele should always be investigated in these patients.
When is varicocele usually detected?
Varikoceles are typically detected due to one of the following reasons:
- Most commonly, they are detected in men with no symptoms whatsoever during infertility evaluations.
- A lump in the scrotum may be noticed by the patient or doctor during a routine examination.
- The patient may consult a doctor due to discomfort, fullness, or pain in the testicle and scrotum areas.
What Kind of Pain Can Varicocele Cause?
Discomfort, fullness, or pain may develop in the testicle and scrotum areas due to varicocele.
Patients often describe a painful sensation in the testicular region, which is usually associated with prolonged standing or activity. The discomfort often decreases when lying on one's back with the legs elevated.
The evaluation of patients with pain should include scrotal ultrasound to rule out other pathologies and a urine test to rule out infection.
When no other cause of pain is found and the characteristics of the pain are consistent with varicocele, varicocele surgery may be considered, but it cannot be guaranteed that varicocele repair will completely eliminate the pain.
In patients scheduled for varicocele surgery solely due to scrotal pain,
microscopic denervation of the nerves of the spermatic cord may also be considered during surgery.
The Relationship Between Varicocele and Male Infertility
Varicocele is detected in approximately 40% of men who consult a doctor for fertility issues.
This means that varicocele can be detected in 4 out of every 10 men. This indicates that varicocele is one of the most common causes of male infertility.
Varicoceles are classified according to their degree (mild, moderate, severe) and whether they are unilateral or bilateral.
However, it is important to note that varicoceles can have a negative effect on fertility regardless of whether they are low or high grade.
In other words, not only high-grade varicoceles but also low-grade varicoceles can impair sperm production and quality.
Current research has shown that varicoceles can impair not only sperm count and motility, but also sperm function.
These impairments can sometimes occur without any problems being apparent in classic semen analyses. In other words, even if the patient's sperm count appears normal, the sperm may not be able to perform their function properly.
Furthermore, even if varicocele is present in only one testicle, it is known that the other testicle may also be adversely affected due to increased heat and circulatory impairment.
This situation can disrupt both sperm production and hormonal balance.
How is a Varicocele Diagnosed?
The diagnosis is usually made through a urological physical examination. During the examination, the varicose veins of the testicles can be felt when the patient is standing. Colour Doppler ultrasound is used to monitor testicular volume and evaluate vein diameter. This method also measures the amount of blood reflux.
Varicoceles that are detected only by ultrasound and not by physical examination (subclinical) are considered clinically insignificant because they rarely impair testicular function or cause discomfort.
Ultrasound can reveal varicoceles in situations where physical examination is difficult due to the patient's anatomy or when other findings prompt the doctor to request a scrotal ultrasound.
Large varicoceles are often visible to the naked eye, or the patient may notice a "worm-like" sensation in the scrotum.
However, more commonly, varicoceles are only detected during a doctor's examination.
Therefore, the best way to detect a varicocele is through a careful physical examination by a urologist.
Even experienced general urologists may sometimes be uncertain about the diagnosis, so an ultrasound should be performed if there is any doubt.
Varikocele Treatment
Varikocele treatment is determined based on the patient's complaints and plans for having children. Treatment is generally not required for men who have no complaints and do not plan to have children; regular follow-up is sufficient.
Surgical treatment is used in cases where there are complaints or where infertility is associated. The most common method today is microscopic varicocelectomy. In this operation, the dilated veins are tied off to allow blood to return through normal channels.
Untreated varicocele may increase the risk of infertility in some individuals. In addition, testicular volume loss (atrophy) and chronic discomfort may develop. After surgery, hydroscele formation or recurrence of varicocele may occur, albeit rarely.
When Should Varicocele Be Operated On?
The decision to treat varicocele is based on:
- The size of the varicocele,
- The patient's fertility goals,
- Symptoms of low testosterone or scrotal discomfort,
- Blood tests for testosterone and/or semen analysis results.
Additionally, the age and fertility of the patient's female partner are also very important when deciding on varicocele treatment.
If the female partner has not yet been evaluated, she should undergo basic tests to ensure there is no condition that could alter varicocele management.
There is strong evidence for varicocele repair to preserve and improve testicular function before it deteriorates further over time; however, this is closely related to the size of the varicocele.
Therefore, testicular function should be assessed directly through semen analysis, testicular volume measurement, and/or blood tests.
If there is evidence of damage to the testicle, varicocele repair may be important to improve testicular function and/or prevent further deterioration.
If the testicle appears unaffected by the varicocele, there are differing opinions on whether the varicocele should be treated.
If you wish to have varicocele surgery to preserve future testicular function, it is important to discuss this in detail with your surgeon and to be aware of your chances of obtaining a measurable benefit and the risks of side effects from the procedure.
The most important point here is that treatment should only be recommended when this "risk-benefit ratio" is appropriate.
As an alternative to treatment, patients with varicocele can be monitored over time;
for which regular semen analysis, blood tests and ultrasound follow-ups are performed, and treatment is only administered when there is evidence that the varicocele is impairing testicular function.
In a couple experiencing infertility, varicocele repair in the male partner is indicated in the following situations:
- If there is objective evidence of male factor infertility (e.g., abnormal semen analysis)
- If the woman's fertility is intact or treatable
- There are no other obvious causes of male infertility (e.g., obstruction, malignancy, or genetic disorder)
How is Varicocele Surgery Performed?
We now perform varicocele surgery in most patients using the microsurgical subinguinal varicocele ligation technique. This approach provides the highest success rate, the lowest complication rate, and virtually eliminates the risk of serious intra-abdominal injury.

Don't delay, let's meet now !
- Feneryolu Bagdat Avenue No 85/1 Postal Code: 34724 Kadıköy/İstanbul - Turkey
How is Microsurgical Subinguinal Varicocele Surgery Performed?
For this procedure, the patient is put under general or spinal anaesthesia. A small incision is made in the lower groin area, and the structure called the spermatic cord, which contains the veins and channels leading to the testicle, is carefully isolated.
Then, the dilated veins are located and tied off under a microscope, thus preventing blood from flowing back from the testicle. Structures important for testicular function are preserved.
Why Should Subinguinal Microsurgery Be Performed?
The subinguinal approach prevents the cutting of muscle fibres, which leads to reduced post-operative pain and a lower risk of hernia. The use of state-of-the-art surgical microscopes during this procedure
allows for careful preservation of important structures and ligation of only the veins contributing to varicocele.
This helps prevent potential post-operative complications (e.g., hydrocele).
How many days do you stay in hospital after microsurgical subinguinal varicocele surgery?
Microsurgical varicocelectomy is often an outpatient procedure, so patients are usually discharged on the same day.
What Are the Complications of Varicocele Surgery?
- Persistent/recurrent varicocele
- Bruising in the scrotum and surgical area
- Infection
- Testicular sensitivity
- Hydrocele: Fluid accumulation around the testicle (hydrocele) may occur in a very small number of patients.
Varikosel Onarımı Doğurganlığı Nasıl Olumlu Etkiler?
Varikosel ameliyatı, çocuk sahibi olma şansını önemli oranda arttıran bir tedavi yöntemidir.
2. derece varikoseli olan ve kısırlık nedeniyle takip edilen 540 erkekte yapılan önemli bir çalışmada, mikrocerrahi varikoselektomi sonrası hastalar 1 ve 2 yıl boyunca izlenmiştir.
Çalışmanın sonuçları oldukça dikkat çekicidir:
- Toplam hareketli sperm sayısında %50’den fazla artış, hastaların yarısında (271 kişi) görülmüştür.
- Ortalama 7 ay içinde (1–19 ay arası) hastaların %36,6’sında eşleri kendiliğinden hamile kalmıştır.
- Daha önce tüp bebek (IVF/ICSI) önerilen hastaların %31’i, ameliyat sonrası artık aşılama (IUI) ile çocuk sahibi olabilecek duruma gelmiştir.
- Aşılama adayı olan erkeklerin %42’si, ameliyat sonrası doğal yolla çocuk sahibi olma şansına ulaşmıştır.
Bu sonuçlar, mikrocerrahi varikosel ameliyatının sperm kalitesini belirgin şekilde iyileştirebileceğini ve doğal yolla gebelik ihtimalini artırabileceğini göstermektedir.
Ayrıca, bu ameliyat sayesinde bazı çiftlerin tüp bebek gibi ileri üreme yöntemlerine olan ihtiyacı azalabilir.
Varikosel Ameliyatı Testosteron Üretimini Etkiler mi?
Testisler, hem sperm hem de erkeklik hormonu olan testosteronu üretir. Varikosel, bu damarların genişlemesine ve testislerin ısısının artmasına yol açtığı için, testislerin çalışmasını yavaşlatabilir.
Bazen bu durum, testosteron seviyesinin düşmesine de neden olabilmektedir.
Ameliyatla varikosel düzeltildiğinde ise, çoğu erkekte testosteron üretimi toparlar ve hormon seviyesi yükselir.
Bu artış özellikle, ameliyat öncesinde testosteron seviyesi düşük olan erkeklerde daha belirgin olarak gözlenmektedir.

